On September 29, Eleanor Beatrice and Adam Ross were born. They were only 23 weeks 4 days gestation, but had to be born because of an infection I had called chorioamnionitis. I was given intervenous antibiotics and antifungal medication for several days, but it did not clear up the infection. It may have given me a few days, though, in which the doctors could administer steroids to me that helped accelerate the development of the lungs in the babies. The neonatologists visited us in the days before they were born telling us that babies born at this gestation only had a 30 percent chance of survival. This was obviously devastating, and we had made plans for the worst. When they were born, there were at least 30 people in the delivery room who whisked Adam and Eleanor to the Neonatal Intensive Care Unit immediately. Unfortunately, I didn't get to see them before they had to go.
When I fist saw them, they were hooked up to many IVs and to ventilators, and inside isolettes set to 75% humidity. They looked very tiny, very red, and absolutely perfect. I know to the few people who saw them then, they may not have looked like the beautiful babies people are used to seeing at the hospital, but they were absolutely gorgeous to me. While I was still admitted to the hospital, I went to see them all the time. When I was discharged, I came in around 7am and left around 11pm. I couldn't leave them for a minute not knowing what was going to happen next.
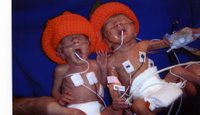 The neonatologists immediately did blood cultures on the twins to find out if the infection from me had been transferred to them. Oddly enough, it hadn't been, although Eleanor had a different infection called serratia. She was on many antibiotics for this. Anyone who has been through the NICU experience will tell you that just as one thing is looking good, they tell you something new that your babies will have to overcome. After one week in the NICU, both twins had to have a cranial ultrasound. This was to determine if they had any IVH (intraventricular hemmorrage or brain bleeds) which are so common in premature infants, particularly those born under 1000 grams. This is when we started to realize just exactly how miraculous our babies were. Neither of them had any bleeds at all!! This was such a major milestone since bleeds, depending on their severity, can cause cerebral palsy, deafness, blindness, and a condition called PVL where part of the brain essentially dies, just for example. We soon learned about PDAs. A PDA (patent ductus arteriosis) is a duct between the pulmonary artery and pulmonary vein that usually closes at birth. For babies born too early, this doesn't happen. They gave both babies a medication called indocin to close the duct. It worked for Adam, but not for Eleanor. She had to have surgery to fix this problem. Then, when the surgery was scheduled, we had to cancel twice and postpone because her infection had not yet gone away. A wonderful woman, a pediatric pharmacologist (I didn't even know there was such a thing before this) did a sensitivity test and gave Eleanor Amacacin (sp?) Much later, she told me it was the first time they had used this medication at our hospital in the NICU. Yikes!! But it worked. On the day of the surgery in October, Eleanor's eyes, which had been fused since birth, finally opened completely. As she was put in the transporter to be taken to the operating room, she looked right at me. All I wanted to do was take her out of there and hold her, but I knew the surgery had to be done. It only took about an hour and a half from beginning to end, though it seemed like forever. In the days following the surgery, Eleanor's status declined. She had difficulty maintaining her blood pressure and ended up on the oscillating ventilator. She was on dopamine and debutamine for her blood pressure and the decided to give her a steroid, hydrocortisone, to improve her respiration. After a few days, she started to improve and the blood pressure meds were taken off. She stayed on the hydrocortisone for about a week and a half, and in that time she came of the vents and went on to CPAP. CPAP is a breathing apparatus that supplies continuous pres
The neonatologists immediately did blood cultures on the twins to find out if the infection from me had been transferred to them. Oddly enough, it hadn't been, although Eleanor had a different infection called serratia. She was on many antibiotics for this. Anyone who has been through the NICU experience will tell you that just as one thing is looking good, they tell you something new that your babies will have to overcome. After one week in the NICU, both twins had to have a cranial ultrasound. This was to determine if they had any IVH (intraventricular hemmorrage or brain bleeds) which are so common in premature infants, particularly those born under 1000 grams. This is when we started to realize just exactly how miraculous our babies were. Neither of them had any bleeds at all!! This was such a major milestone since bleeds, depending on their severity, can cause cerebral palsy, deafness, blindness, and a condition called PVL where part of the brain essentially dies, just for example. We soon learned about PDAs. A PDA (patent ductus arteriosis) is a duct between the pulmonary artery and pulmonary vein that usually closes at birth. For babies born too early, this doesn't happen. They gave both babies a medication called indocin to close the duct. It worked for Adam, but not for Eleanor. She had to have surgery to fix this problem. Then, when the surgery was scheduled, we had to cancel twice and postpone because her infection had not yet gone away. A wonderful woman, a pediatric pharmacologist (I didn't even know there was such a thing before this) did a sensitivity test and gave Eleanor Amacacin (sp?) Much later, she told me it was the first time they had used this medication at our hospital in the NICU. Yikes!! But it worked. On the day of the surgery in October, Eleanor's eyes, which had been fused since birth, finally opened completely. As she was put in the transporter to be taken to the operating room, she looked right at me. All I wanted to do was take her out of there and hold her, but I knew the surgery had to be done. It only took about an hour and a half from beginning to end, though it seemed like forever. In the days following the surgery, Eleanor's status declined. She had difficulty maintaining her blood pressure and ended up on the oscillating ventilator. She was on dopamine and debutamine for her blood pressure and the decided to give her a steroid, hydrocortisone, to improve her respiration. After a few days, she started to improve and the blood pressure meds were taken off. She stayed on the hydrocortisone for about a week and a half, and in that time she came of the vents and went on to CPAP. CPAP is a breathing apparatus that supplies continuous pres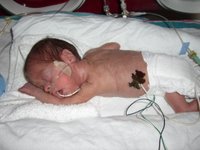 sure into the lungs to keep them open, but Eleanor was now breathing on her own. In the photos, CPAP is the mask/tubes on their faces. It looks worse than the vents, but is actually much better for the lungs. Since the CPAP caused too much air to go into her digestive system, the neonatologists decided to put her on a nasal cannula as a trial. She did so well on it that they never took her off! Of course, she had lots of desaturations (not enough oxygen in her blood)and her oxygen levels had to be turned up, but we were all patient with her and she did fine. By this time, they started feeding Eleanor little tiny amounts of food. It had been a scary month, but looking back, this is when things really started to take off for Eleanor.
sure into the lungs to keep them open, but Eleanor was now breathing on her own. In the photos, CPAP is the mask/tubes on their faces. It looks worse than the vents, but is actually much better for the lungs. Since the CPAP caused too much air to go into her digestive system, the neonatologists decided to put her on a nasal cannula as a trial. She did so well on it that they never took her off! Of course, she had lots of desaturations (not enough oxygen in her blood)and her oxygen levels had to be turned up, but we were all patient with her and she did fine. By this time, they started feeding Eleanor little tiny amounts of food. It had been a scary month, but looking back, this is when things really started to take off for Eleanor.Even though the medication to close Adam's PDA worked, he had a series of other problems. His lungs were just not as mature as Eleanor's. Believe it or not, they call white preemie boys, "Wimpy White Boys." This is because of all races and both sexes, white boys always do the worst. I don't know the explanation for this, but it is true. Adam's respiratory status continued to decline. He was on the oscillating ventilator. The most disturbing part of this vent is that they had to, in essence, paralyze him to make it work. Adam was given a drug called Pavulon, along with morphine, so that he would stop breathing for himself altogether and the oscillating vent could "shake" the oxygen into his lungs and "shake" the carbon dioxide out. Even on this vent with all these meds, his oxygen needs were up to 100%, and his blood oxygen satuarations were still not meeting the minimum. Finally, Adam
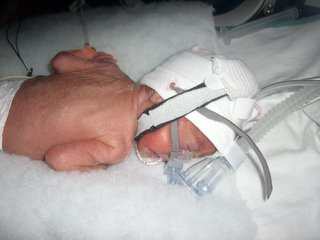 had to be given a steroid called dexamethazone. It is a controvesial drug today because it has been shown, when used over a long periods of time, to cause cerebral palsy, but at this point, we really had no choice. It also can weaken the immune system. It didn't work immediately, but after a few days, it was amazing to see how much better Adam was doing. He came off the oscillating vent (thank God--that was horrible to see him not able to move), went onto the traditional vent, and then after awhile to CPAP. WIth all good things in the NICU come the bad. Adam's heart rate was going up and the doctors could hear a murmur, so they did an echocardiogram. By this time, Adam had had several to make sure his heart was formed correctly. In the echo, it showed that the dexamethazone created a side effect called cardiomyopathy. Basically, the walls of his ventricles were thickening so very little blood was able to be pushed through the heart in one pump, so the heart had to pump faster to keep up. The doctor who read the echo said to stop the steroids immediately and put Adam on enderol. The enderol lowered his heart rate and caused the cardiomyopathy to dissapate. This took about a week, and when they came back to do another echocardiogram, there was marked improvement. Another week or so and the enderol had fixed the problem. Adam remained on a small dose of enderol for quite awhile. Repriatory-wise, Adam had to remin on the CPAP. They did many, many blood gasses to detect whether he was getting enough oxygen into his blood and enough carbon dioxide out. He retained fluid, particularly in his lungs, but even in his face which swelled up quite a bit. I always felt sorry for him because he looked so uncomfortable. He was given diuretics which got rid of the excess fluid and helped him to breathe better. When things seemed to be going well, they tried Adam on the nasal cannula for one hour at a time. He had to be on high oxygen settings, but it was great to be able to see his face under that CPAP mask. Unfortunately, Adam had a bad gas test done where his carbon dioxide was quite elevated, so he had to be reintubated (put back on the ventilator). His lungs had collapsed again, so the vent would help open them up. It was a terrible experience because he hated the vent so much and was so uncomfortable. We couldn't even peek under the blanket over the isolette to look at him because he would get upset and the monitor would show he was desatuarating again. I thought we were out of the woods before that, but we weren't, and we hit the bottom of the NICU rollercoaster again. After a day or two, Adam improved dramatically, but they kept him on the vent for about 5 days to gain strength. Luckily, Adam was able to continue eating except for one or two feedings, during this time. After 5 days, Adam decided that was enough and extubated himself (pulled the vent tube out of his throat). He went back on CPAP and that was the last we had to see of the vents. During all of this at some point, it was discovered that Adam also had the same infection Eleanor had earlier. He was given the same medication and it cleared up. Adam had a knack of taking 5 days for blood cultures to grow anything, when most times they should grow in 48 hours. I never believed a negative blood culture for at least a week! One of the first things one of the doctors had told me when they were born is that infection would be the life or death of Adam and Eleanor. That thought never once left my mind.
had to be given a steroid called dexamethazone. It is a controvesial drug today because it has been shown, when used over a long periods of time, to cause cerebral palsy, but at this point, we really had no choice. It also can weaken the immune system. It didn't work immediately, but after a few days, it was amazing to see how much better Adam was doing. He came off the oscillating vent (thank God--that was horrible to see him not able to move), went onto the traditional vent, and then after awhile to CPAP. WIth all good things in the NICU come the bad. Adam's heart rate was going up and the doctors could hear a murmur, so they did an echocardiogram. By this time, Adam had had several to make sure his heart was formed correctly. In the echo, it showed that the dexamethazone created a side effect called cardiomyopathy. Basically, the walls of his ventricles were thickening so very little blood was able to be pushed through the heart in one pump, so the heart had to pump faster to keep up. The doctor who read the echo said to stop the steroids immediately and put Adam on enderol. The enderol lowered his heart rate and caused the cardiomyopathy to dissapate. This took about a week, and when they came back to do another echocardiogram, there was marked improvement. Another week or so and the enderol had fixed the problem. Adam remained on a small dose of enderol for quite awhile. Repriatory-wise, Adam had to remin on the CPAP. They did many, many blood gasses to detect whether he was getting enough oxygen into his blood and enough carbon dioxide out. He retained fluid, particularly in his lungs, but even in his face which swelled up quite a bit. I always felt sorry for him because he looked so uncomfortable. He was given diuretics which got rid of the excess fluid and helped him to breathe better. When things seemed to be going well, they tried Adam on the nasal cannula for one hour at a time. He had to be on high oxygen settings, but it was great to be able to see his face under that CPAP mask. Unfortunately, Adam had a bad gas test done where his carbon dioxide was quite elevated, so he had to be reintubated (put back on the ventilator). His lungs had collapsed again, so the vent would help open them up. It was a terrible experience because he hated the vent so much and was so uncomfortable. We couldn't even peek under the blanket over the isolette to look at him because he would get upset and the monitor would show he was desatuarating again. I thought we were out of the woods before that, but we weren't, and we hit the bottom of the NICU rollercoaster again. After a day or two, Adam improved dramatically, but they kept him on the vent for about 5 days to gain strength. Luckily, Adam was able to continue eating except for one or two feedings, during this time. After 5 days, Adam decided that was enough and extubated himself (pulled the vent tube out of his throat). He went back on CPAP and that was the last we had to see of the vents. During all of this at some point, it was discovered that Adam also had the same infection Eleanor had earlier. He was given the same medication and it cleared up. Adam had a knack of taking 5 days for blood cultures to grow anything, when most times they should grow in 48 hours. I never believed a negative blood culture for at least a week! One of the first things one of the doctors had told me when they were born is that infection would be the life or death of Adam and Eleanor. That thought never once left my mind.From that point on, we mostly watched them for another problem (one more leaflet, I would always say) called NEC. NEC is necrotizing entrocolitis, a disease where part of the bowel can bleed and die, or create a hole causing infection. Infections of all kinds are serious to preemies, and if the problem is bad enough, surgery would have to be done to remove the affected portion of the bowels. It can cause many problems, including death.Since preemies this small should not yet have had actual food in their digestive system, they weren't ready for it. They must be fed, though, in order to grow and heal from all the other issues. So we watched carefully for any signs of bloating, discoloration of their stomachs, and for "risidual", or aspirate. Since they were being fed through OG tubes (tubes down their mouths into their stomachs) the nurses could , after three hours, use a syringe to suck back up anything left in their stomachs. The idea is that they digested all the food they were given and the stomach should be empty. At first, the milk irritated their stomachs and there would sometimes be risiduals. If it was just a little, it wasn't a problem. If there was more that 20%, the doctors were informed. A couple times they did x-rays (they must have had 50 each on their lungs, let alone their absomens) to make sure there weren't problems, but for the most part, the scariness of NEC passed without too many issues. I called those poor nurses every three hours during the nighttime feeding, though, for weeks to find out about risiduals, making sure that Adam and Eleanor were doing well. They only teased me a little bit!
Once the feedings were going well, and the twins started holding their own temperatures better, the decided to move them to a crib where they could be bundled together. This was a big move for me--I like them all safe and sound in their isolettes--but it was great for them. It seemed that they had missed each other for the last 2 1/2 months while they were separated. They "failed the crib" the first time, meaning they couldn't keep their temperatures up, but did fine about a week later when they had gained some more weight. On average, the doctors like to see preemies gain about an ounce a day. Adam was still on the CPAP, but they were adding nasal cannula time gradually, so that he was on it 2 hours a day, then 4, then 6, etc. Once he was able to stay on the cannula full time, they moved us from our little corner in the back of the NICU to the front room where there is less intensive care. At first Adam and Eleanor each had their own nurse. Then they shared a nurse. Now there was one nurse for them plus one or two other babies. This is when we were really able to relax a little (though some certain NICU nurses might get a giggle out of the thought that I was ever "relaxed.")
During this time, a pediatric opthamologist started seeing Adam and Eleanor. It is typical for babies born at their gestation to have a problem with their eyes called ROP (retinopathy of prematurity). This is where the immature blood vessels of the eyes don't grow properly, cause ridges within the eye, and if not watched carefully, can cause blindness from detached retinas. There are many thoughts as to why this happens, including high levels of oxygen administered though ventiliators. We assumed when the doctor came that both of them would need laser surgery to correct thie eyes--particularly Adam because of the amount of oxygen he had required. They were seen once a week while in the NICU. Neither Adam nor Eleanor have ended up with any ROP that will require surgery. Eleanor's has resolved itself completely already, and Adam is close.
On December 5, 2005 Eleanor got to try bottle feeding for the first time. It was a great day for both of us! The nurse prepared me by saying that she may not take much and she will probably choke, etc...but Eleanor surprised us and took the whole bottle. She had decided she wanted to get out of the NICU and fast! It took awhile for her to have enough energy to eat from the bottle every time, but once she did, that nasty tube was taken out of her nose and she was eating everything by mouth--or "PO" as the nurses would say. About a week or so later, Adam tried bottle feeding. He didn't do so well right off the bat, but he improved gradually. It took him until 3 days before we left the NICU to take everything by bottle. You wouldn't know it now, the little guy eats so much! During this time, the doctors weaned Adam from all of his medications. It took awhile, but both were just on vitamins by the time we left the NICU.
The last few things that had to be done before discharged were now reviewed with us. There were hearing screens which they both passed--though Adam had to do his twice. Both twins had an MCR, or sleep study done. It showed that they would each go home on 1/4 liter oxygen and apnea monitors. They also had to do a car seat test to make sure they would be able to be in the car seat and not have breathing issues. Once that was complete and they were taking all their feedings by bottle we were out the door. It was a bittersweet day. The doctors and nurses at our hospital were amazing. They became our second family, and our friends. There were decisions made daily, even hourly, that saved Adam and Eleanor's lives over and over again. Along with the many hours of prayers said for our two little miracles, there were doctors who cared as if they were taking care of their own children, nurses who remembered every medication, every change of tubing, every feeding, and noticed even the most subtle changes in own children, and repiratory therapists who, even under the most stressful situations, gave Adam and Eleanor exactly what they needed to continue breathing. Adam and Eleanor are far from the typical 23-week baby. Jim and I understand what amazing miracles our babies are--they have no IVH, no hearing problems, no vision problems, no eating problems. They are, so far, great at gaining weight. We don't know what the future holds for Adam and Eleanor. They may have other, more subtle disabilities as they grow up, but it seems to me that they will be able to accomplish whatever it is they want to in this world, seeing what they have accomplished already. I so admire their persistence and tenacity. We are amazed by them every single day.